
Bowing
Parents of children who have bowed legs often want to know if the child's legs are abnormal. To help answer that question, here are some basic facts about bowing. This section will give you an idea of what the physician is thinking about when he or she is examining your child.
First, bowing or the technical term genu varum (genu = knee, varus / varum = angles in) is a part of the normal development of a child. The role of the physician is to determine if the bowing is physiologic (part of normal development) or pathologic (due to some disease process). Physiologic bowing will improve as the child grows without treatment, while pathologic bowing will tend to worsen over time without treatment. The bowing can arise from the lower portion of the femur near the knee, the knee joint itself, the upper shin bone near the knee, or a combination of these areas.
Normally, an infant is born with bowed legs. Over time, the leg alignment will correct and usually straightens out by about eighteen months of age. By the
time the child is three to four years old, he or she will normally develop a knock-kneed alignment. The technical term for this is genu valgum (valgus/valgum = angles out)
. This genu valgum will then correct somewhat by the age of five to six years old, leaving the normal adult alignment of slight genu valgum (slight knock-kneed).
Listed above are the mean ages for these
changes to occur so half of the children will correct their bowing earlier and half will correct it later. Occasionally, the bowing never fully corrects. That is why some adults have bowed legs. So you can
see, there is a wide range of normal when looking at bowed legs. Physiologic bowing does not require any treatment other than observation for correction as the child grows.
Internal tibial torsion (inward twist of the tibia caused by intrauterine positioning), also called medial tibial torsion, can complicate matters by making the bowing appear worse than it really is, as we see the side of the knee relative to the foot rather than the front. Correction of the torsion will make the legs appear straighter. Fortunately, internal tibial torsion tends to correct itself without treatment up until the age of four to six years, thereby correcting the visual bowing also.
Many disease processes effecting bone growth cause pathologic bowing. Two of the more common diseases known to cause bowing are Rickets and Blount's disease.
Rickets:
Rickets is a generalized skeletal disease involving Vitamin D
metabolism. Vitamin D is vital for bone mineralization. Although this vitamin is important it does not act alone. The term 'rickets' predates the later and current notions of the actual causal chemistry. So older usage's run counter to current more precise etiologic (based on cause) uses of the term. In the older sense, a child with bowing of bones, with thickened ends of bones (including ribs), often irritable, and eventually (when x-ray allowed) noted to be associated with widened growth plates which did not fully calcify - that was called rickets. Calcium as Ca++ interacts with Phosphate as PO4= such that at a certain concentration, the calcium can precipitate. The body uses several mechanisms to keep the two at a certain level. When that is off - either by the Ca++ or by the PO4= then the syndrome may manifest.
Dietary deficiency of Vitamin D is the most familiar (to the public) form of rickets. Dietary supplementation of Vitamin D has gone a long way toward abolishing dietary rickets, but it still occasionally seen in less developed countries and in circumstances of dietary peculiarity. Because of this, the hereditary forms of rickets are more commonly seen. Rickets causes a distinctive cupping and widening of the growth plates which can be recognized on a plain x-ray along with other characteristic findings.
However, rickets, in today's terminology, is really a family of entities. Vitamin D in the diet isn't really an active agent, but rather a precursor, a build it yourself kit for what is often called "active vitamin-D". The substance in the diet must first be absorbed, altered by the liver, then altered further by the kidney, then changed again in the skin by sunlight before it is in the active form. If any of those steps is faulty, then dietary vitamin D will be no more active than sand or jelly beans.
Therefore, even with a normal intake of "vitamin-D", if any of the needed bodily steps are not functional, a rickets syndrome may be seen. Caught early, while there is lots of growth remaining, corrected growth can undo deformations which have not gone too far. Correction by supplements is from corrected growth. No growth, no correction. Adults will not correct bowed bones by diet.
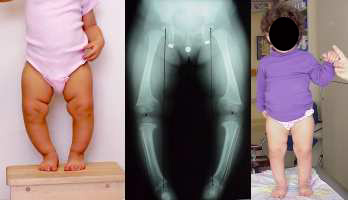 The little girl on the right has a
genetic form of rickets seen only in the females of her family (four generations). A dominant defective gene disabled her ability to activate the vitamin D form found in food. Dietary change would do little.
The little girl on the right has a
genetic form of rickets seen only in the females of her family (four generations). A dominant defective gene disabled her ability to activate the vitamin D form found in food. Dietary change would do little.
At an early time, by giving her a processed already activated form of vitamin D which gets around her inherited bodily inability to activate it, her deformities went away. Her younger sister with similar findings behaved in exactly the same manner. Although boys in alternate generations could also land this particular gene defect, four generations in this girl bearing family managed to dodge this outcome. The girls treated early have statures greater then mother, grandmother and great grandmother by age 8.
Active vitamin supplementation will not undo deformities if they are addressed too late for remaining corrective growth to get the job done. If the activated form of
the vitamin fails to alter the course of things then rather than blame the key (vitamin D) we need to suspect the lock. Hormones or vitamins work like keys by
fitting into something that responds. If that something is defective, then it gets even more difficult to get around.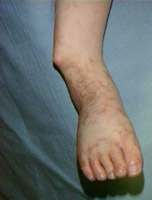 On the left we see an extreme form of rickets with multiple tiny fractures caused by a defect in the mechanism which uses
vitamin D, that is there is no deficiency of the vitamin or the activated form. Odd metabolic work around tricks are required when this occurs. This form of rickets has
interaction with zinc, magnesium, and interestingly, growth hormone. In genetic disorders, it is not uncommon that a so called something defect actually involves more than the
something that names it, as deep biochemical alterations often have broad, metabolic echoes.
On the left we see an extreme form of rickets with multiple tiny fractures caused by a defect in the mechanism which uses
vitamin D, that is there is no deficiency of the vitamin or the activated form. Odd metabolic work around tricks are required when this occurs. This form of rickets has
interaction with zinc, magnesium, and interestingly, growth hormone. In genetic disorders, it is not uncommon that a so called something defect actually involves more than the
something that names it, as deep biochemical alterations often have broad, metabolic echoes.
The complexity of the treatment of rickets varies with the complexity of the curvatures. Most cases are treated with medicine alone, but extreme cases, such as the one above, require surgical correction.
Blount's Disease: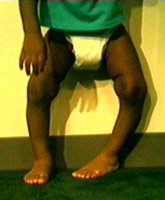 Blount's disease affects the inner edge of the upper shin bone at the knee growth plate (epiphyseal plate - runs
horizontally across the knee), causing it to decrease its rate of growth in the portion of the growth plate that is closest to the leg's inseam. The outside part of the growth plate continues to grow normally, leading to
progressive bowing.
Blount's disease affects the inner edge of the upper shin bone at the knee growth plate (epiphyseal plate - runs
horizontally across the knee), causing it to decrease its rate of growth in the portion of the growth plate that is closest to the leg's inseam. The outside part of the growth plate continues to grow normally, leading to
progressive bowing.
Blount's disease affects two different age groups. There is infantile Blount's, seen in young children, and adolescent Blount's, seen in teenagers. In both groups, the children tend to be overweight for their age. This bowing deformity is always associated with internal tibial torsion (an inward direction of the ankle and foot relative to the direction of the knee - see above picture). The left knee, above, is aimed dead straight ahead, yet the ankle is directed toward the child's right.
If infantile Blount's is diagnosed early enough,
bracing can be instituted. We have had good results bracing children as young as two years old. Usually by the
age of three, treatment will require a tibial osteotomy (surgery of the tibia) to straighten the lower extremity. Many will wait and "see how it goes", and let the
most effective bracing period go right by. In a special parallax-free three exposure x-ray of the full leg from hip to ankle, with the knee carefully aimed straight ahead
, a line through hip and ankle centers ought to pass through knee center. If that line passes outside the bone of the knee, then the angulation will worsen with time
and not self-correct. We have seen no such reversals in that subset of children. We prefer to brace as bracing early not only works better but heads off the
addition damage to the inner growth plate caused by the angular mechanical (nut cracker) compression caused by the bowed leg.
Depending on how crushed the growth plate is, the bowing may recur
after surgery. Tibial osteotomy (tibia = shin bone, osteo = bone, tome = to cut) is also part of the treatment for the adolescent. There are many different techniques for
performing the osteotomy. No matter what technique is chosen, the osteotomy must correct the bowing and twist (tibial torsion) at the same time. Bracing also attempts to correct both deformities at the same time.
X-rays are helpful for diagnosing Blount's disease as well. But there is an important detail to be aware of when taking these x-rays. Usually an anterior -posterior (AP) view of the lower extremity is obtained with the knee pointed straight ahead (ignoring the foot direction). The growth plates are checked for any abnormality, such as is seen in rickets and other diseases. Angle measurements about the proximal tibia as well as between the tibia and femur are made, which will help determine if Blount's disease is present. Importantly, a line from the center of the hip joint to the center of the ankle joint is drawn as discussed above. This is the best prognosticator for progression.
This line is the weight bearing line of the lower extremity. If it passes completely
beyond the knee joint substance, then whenever weight is placed on the leg it is passed from the hip to the ankle levered through the very medial part of the knee.
The leverage amplifies the forces. This will tend to make the bowing worse over time, damaging the growth plate, and is an indication for treatment of the bowing.