 In the embryology section we looked into the early growing structure to see the narrow strip of ectoderm neural tissue begin to 'tubulate' by
zippering into a tube from middle to up and down. The neural crest cells sit right on the edge of that zipper adjacent the developing mesoderm deep to the rest of the ectoderm
(destined to be skin) not shown here (peeled away - oooooooo - yuk). Just pictures. No actual ectoderms were harmed in the making of this discussion.
In the embryology section we looked into the early growing structure to see the narrow strip of ectoderm neural tissue begin to 'tubulate' by
zippering into a tube from middle to up and down. The neural crest cells sit right on the edge of that zipper adjacent the developing mesoderm deep to the rest of the ectoderm
(destined to be skin) not shown here (peeled away - oooooooo - yuk). Just pictures. No actual ectoderms were harmed in the making of this discussion.
The neural crest becomes the link (peripheral nervous system) between the central tube (the central nervous system) and the and everything else practically. In the segmented tissues, the somites will become various things including muscles.
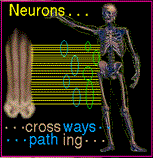 See? Those yellow connections, the neural crest, has a perfectly orderly bead on those
somites so everything is connected straight away. But as ships going to sea and far away ports dragging those connections, it gets messy. The rootlets need to be bundled in groups
to pass BETWEEN important developing structures. On the average they take certain paths. On the average. But just like you taking a different road to get home (same starting
and ending place but different route) the nerves which are the grouping of many already connected rootlets become recognized entities but the travelers within may vary a bit. So
the leg pain called 'L4' may indeed be traveling along L3 or L5 in about 10% of cases. This image from the brachial plexus lecture also shows this complexity. People vary. You
knew THAT! But they really vary a lot even at the lowest deepest levels.
See? Those yellow connections, the neural crest, has a perfectly orderly bead on those
somites so everything is connected straight away. But as ships going to sea and far away ports dragging those connections, it gets messy. The rootlets need to be bundled in groups
to pass BETWEEN important developing structures. On the average they take certain paths. On the average. But just like you taking a different road to get home (same starting
and ending place but different route) the nerves which are the grouping of many already connected rootlets become recognized entities but the travelers within may vary a bit. So
the leg pain called 'L4' may indeed be traveling along L3 or L5 in about 10% of cases. This image from the brachial plexus lecture also shows this complexity. People vary. You
knew THAT! But they really vary a lot even at the lowest deepest levels.
So looking at a nerve without being able to see the source nor the destination can be a bit challenging. HOW to you KNOW that this one rootlet is what it is supposed to be - on the average?
 You zap it!
You zap it!
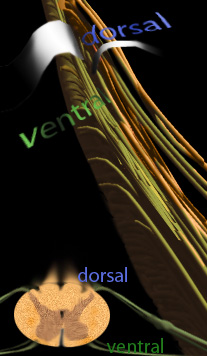
The spinal cord still has those regularly exiting and entering bits of nerve, like teeth on a comb penetrating at tiny intervals. On the back surface (dorsal surface) the sensory nerves form that comb entering.
On the belly side of the cord (ventral surface) the comb of penetrating pathways exit.
Dorsal is sensory - information travels into the cord. Ventral is motor, signals leave the cord. In a short distance, sensory stuff and motor stuff that need to get to and return from the some place have to join up in a common package for that trip (a nerve, a MIXED nerve). Nerves vary in how much sensory and motor information they carry. Some are pure.
At the level we are looking at here, the tiniest sensory and motor bits are already bundled somewhat on leaving the cord then grouped into more structurally sound larger structures before converging on each other to be sorted further out in the bigger anatomy.
So it is here, we can easily (if you know how and go to school for it for 30 years) sort out the sensory roots - free of any motor content. And good news, the sensory stuff is on top as you enter - dorsal.
SDR deals only with sensory nerves (we'll call them nerves as saying rootlets and nerve bits is getting on my nerves).
Terminology: afferent means toward and efferent means away (A=approach, E=exit). So afferent nerves are sensory and efferent nerves are motor. The guys in white coats love to mix these randomly to keep the riffraff confused (that's you). So when they pull that deep speak on you, tell'em to clean it up or you will efferent their office and afferent your home.
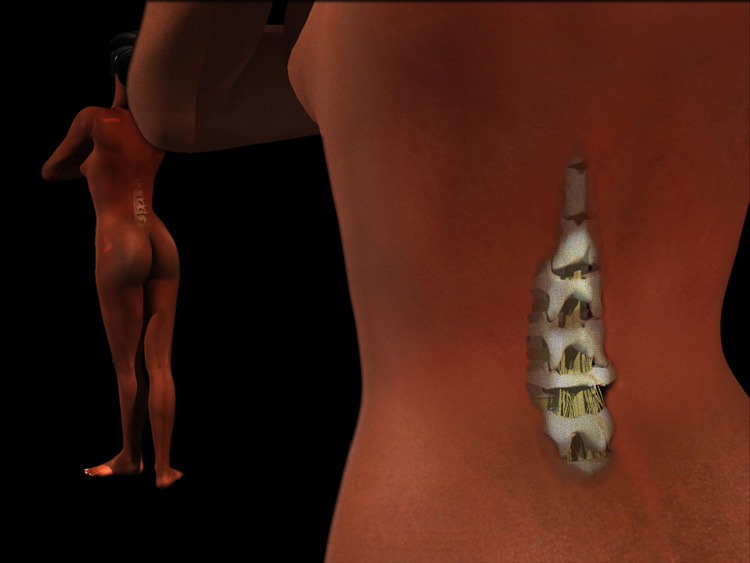 |
OK, so you took the home study course and figured how to in to the spinal canal, and the advanced study guide as to how to peel away the blood vessel carpeted coverings to reveal the many downward traveling roots. The more surface ones are sensory. But which do what? Are they labeled?
No. we already said that we zap them. Each root has to be opened and the tiny - groan - rootlets within need to be splayed gently apart. Then a probe that has a stimulus buzz zaps one rootlet. A physiologist over in the corner is monitoring electrodes that were placed on nerves and muscles.
When you stimulate such a sensory structure the person should say OWWWWWWW! But they are asleep. Every so often a rootlet buzz makes a muscle jump or a nerve somewhere come alive. That is, an in going (afferent) sensory stimulus caused something else somewhere else (efferent) to happen.
Is that BAD? Not a clue, honestly. But if that event goes on and on and on and just drags on then that surely is not good. We assume then that anything coming over this sensory circuit is going into an internal short circuit, This rootlet is cut.
In computer talk we call it GIGO, garbage in garbage out. Here it is GOMMGI. Garbage out must mean garbage in.
THAT, my friends, is SDR!
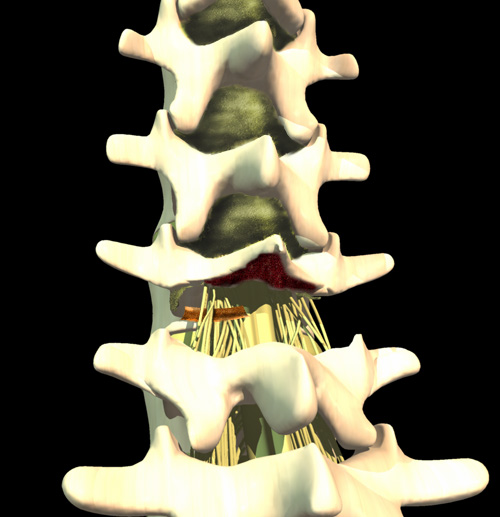 Well, almost. You have 6 more hours of these zillions of rootlets to go. Why do neurosurgeons lack personality? This is why. Who could stand such a repetitive fine motor task that long?
Well, almost. You have 6 more hours of these zillions of rootlets to go. Why do neurosurgeons lack personality? This is why. Who could stand such a repetitive fine motor task that long?
So the 'D' is dorsal. The 'S' is selective, just the ones that don't stop buzzing after stimulated.
What's the 'R'? It's Greek rhizo via an Indo-European root meaning - uh - 'root'. SDR = SDRS selective dorsal root snipping.
Now be careful here. Some folks dressed in white with less patience (? patients?) figure that you could just go in without all that testing and snip a percentage and - on the average - it would be the same! There are always jerks who think that way. They substitute the blurring that averaging causes for the clarity that the art demands. Vote with your feet.
But there are points to be made. The recycling sensory stimulus=>motor output response=>repeat of the same sensory stimulus . . . round & round ... which we call cross firing when it pops up away from the stimulus location - that whole deal is typical of SPASTICITY. The thing that RECYCLES it is the spindle mechanism in the periphery which detects acceleration - speed change. This IS what spasticity is. To the degree that central nervous system damage is confined to ONLY this, then SDR makes sense.
What else? Well those nerves don't physically make circles, the circuits do. One nerve nudging another. But we cam dampen that nudge which is a chemical transmitter nudge by soothing or dampening the nudge points (nerve to nerve junctions). Chloride spilling out does that, and gamma amino butyric acid is a chloride gate opening chemical. GABA ( or something very similar - BACLOFEN - that acts the same but lasts longer) does that. Valium and barbiturates cause the GABA action on the chloride gate to be exaggerated. Unfortunately they also addict, and require escalating dosage and have withdrawal problems - hence Baclofen.
So why dig? Just use Baclofen! But Baclofen is NOT selective. It blunts all GABA related stuff whether short circuited or not - AND - there is also GABA stuff in the brain where its use is totally unrelated and ought not be messed with. To a degree the 'blood brain barrier' helps in that circulating Baclofen may well do the job at the spinal cord at concentrations too low to get through to make trouble in the head. Perhaps, but that is very variable.
So to help the odds, delivering Baclofen directly into the spinal fluid allows a good spinal effect with no mental spill over. Again. spasticity is the target, but Baclofen being a bit less selective does dampen other stuff as well and so may be a better choice when the overactivity isn't spinal local as in RIGIDITY, where the short circuit is in the head. It is less good when the ill is multifocal pure spasticity.
Do all muscles send back high velocity signals? Excluding certain very specialized cases, they all CAN but seldom DO. Why? Because to send back high velocity (actually high change in velocity - acceleration) signals the muscle has to experience it. That experience has to exceed the trip threshold for that receptor. The fact is that the big work muscles have very short excursions and even with all out effort seldom cross that acceleration threshold. The thin surface muscles run further and have very long ranges for those same angular arcs. So mechanically, these are the ones that typically scream over the 'gamma' circuits (the paths that carry the acceleration information). That certain muscles seem to be more spastic is just as much related to their geometry as to central nervous system injury. Spasticity relates to the high speed muscles by threshold velocity not the coincidence of being medial etc. It isn't the WHERE, but the how the muscle is strung.
So attacking high velocity sources at the periphery can also be selective and dampen spastic responses. That's what the S in SPML is referring to.
Down sides to SDR?
Yes a big one and an annoying but easily dealt with one.
Brain damage is like car damage. What's the chances that only a left fender gets smashed. Could happen. But damage can be and typically is more than tightly focal. Sensory damage is as much a part of CP as motor. [Sensory, here, means everything else than motor, so the computing done to use input etc. gets tossed in as well.]
A child who freezes up and seems unable to move while just standing there (yet can push a wheelchair like any other kid) is frozen by lack of input. Hey! LET'S GIVE THIS A NAME! It needs a name or else people jut keep on missing it!
Let's call it SDP - sensory deprived paralysis. I just thought of that. Really. I like it. Use it and pass it on. You have to discriminate CP from the CP variant SDP. Perfect.
Those morons who can't take the long wear-a-diaper SDR sessions - the ones who want to just cut 75% of the sensory rootlets (seriously!) and get the same READINGS on the OUTPUT DEVICE need this terminology to turn them away. Sensory function is measured in motor finesse, not on emg!!!
Recessing a muscle can turn off spasticity in and from that muscle AND create more control from it as it becomes another source of refined input.
The small down side of SDR is that spasticity, per se, responds but fibrosis in certain muscles can and does still occur. That fibrosis is the source of true contracture - loss of range. Secondly, contracture is another source of stimulus to the gamma system (the ones that scream in spasticity). Normal volunteers given an external rig to simulate contracture showed neurologic output that exactly mimicked spasticity. So a kid with SDR can seem to get no improvement if preexisting contracture is there at the time of SDR. Or, the spasticity can SEEM to return when it is really this fibrosis mimicking spasticity. SPMLs or Percs fix this.